Vaccine Q&A: the Logistics of Getting Vaccines to Everyone Who Needs Them
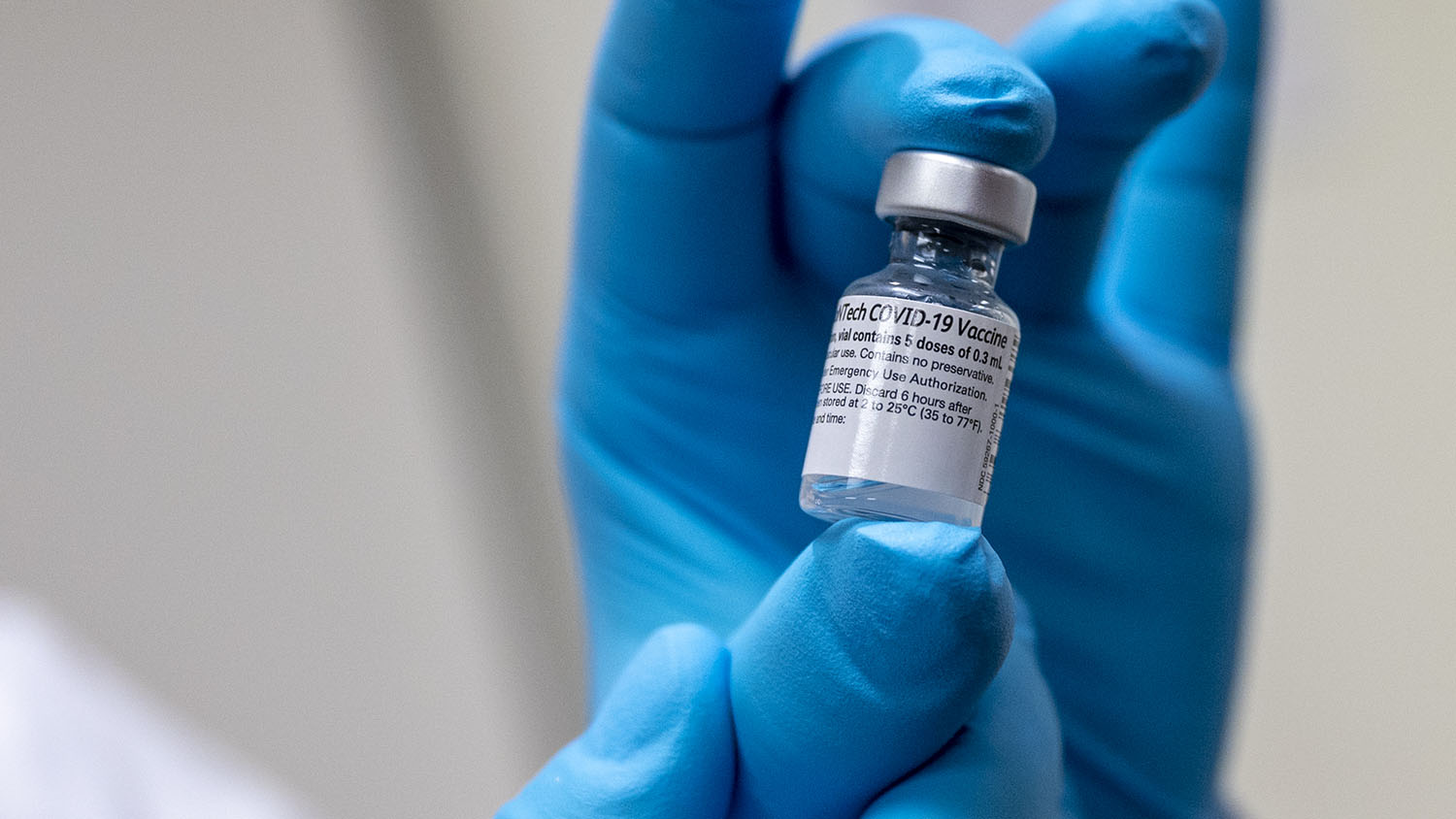
In this post, we focus on the logistical challenges associated with distributing different types of COVID-19 vaccines to millions of people, from urban centers to sparsely populated rural counties.
To address those questions, we spoke with Julie Swann, a systems engineer with expertise in vaccine distribution whose work focuses on making health care and supply chains more efficient, effective and equitable. Swann is the department head and A. Doug Allison Distinguished Professor of the Fitts Department of Industrial and Systems Engineering at NC State.
This post is part of a series of Q&As in which NC State experts address questions about the vaccines on issues ranging from safety to manufacturing to how the vaccines will be distributed. [Editor’s Note: this post has been updated to address a question about the speed of the vaccine rollout. That question is included at the bottom of the Q&A.]
The Abstract: Will vaccines vary from state to state?
Julie Swann: The Pfizer vaccine was approved recently in the U.S. and has started to ship. It is expected that Moderna could receive approval soon with shipments shortly following. I expect both vaccines will go to all states. Once priority populations – such as hospital workers – have been vaccinated, and a larger number of doses becomes available, vaccines will also be sent to commercial pharmacies for distribution. Eventually we may have several more vaccines become available. Consumers may not even realize which they receive unless they have a specific medical condition that is relevant. That said, because these vaccines require two shots, delivered weeks apart, it is important for people to ensure that their second dose is the same type of vaccine as their first dose. This ensures they get the maximum potential immunity from the vaccine.
TA: How much time has to elapse between getting the shots? Why do the vaccines require multiple shots anyway?
Swann: For the Pfizer vaccine, one should have a second shot 21 days after the first. For the Moderna vaccine, the second dose comes 28 days later. This is not unusual, as there are several vaccines where multiple doses are recommended, including for Hepatitis A, Varicella (chicken pox) and others. We have never before had a vaccine for a coronavirus, so it is not surprising that it may take two doses to enable our systems to have full protection. Recently, the data showed that the first dose of Pfizer provided about 50% protection over the next few days, but that it provided 90+% after the second dose.
TA: What are the biggest logistical challenges to distributing the vaccine?
Swann: There are several! We talked about some of these challenges earlier this year.
Some people talk about the scale. For example, it will take approximately 500 million doses to vaccinate a significant portion of the U.S. adult population, because most of the vaccines require two doses. As a comparison, this year we have a supply of 198 million doses of influenza vaccine, and the H1N1 pandemic response distributed more than 100 million doses in emergency settings. So the scale is impressive, but not insurmountable, especially given that the systems will build upon previously used practices.

One challenge is the cold chain that is required, especially for a vaccine like the one from Pfizer, which currently needs to be stored at -70 degrees Celsius (-94 degrees Fahrenheit). That is much colder than our freezer temperatures. Pfizer has developed a special thermal shipping box that can have dry ice added every five days for up to a total of 30 days. Once thawed it should be kept at 2-8 degrees C (refrigeration) for no more than five days. The shipping box contains about 1,000 to 5,000 doses, so it is likely to be more appropriate for cities, or locations that will host mass vaccination clinics.
The Moderna vaccine can be stored at -20 degrees C for months or at 2-8 degrees C for up to 30 days. Those shipments will contain a minimum of 100 doses each, so it may be appropriate for smaller locations, including rural ones. Fortunately, from the initial available data, those two vaccines have similar profiles in terms of safety and efficacy.
A third challenge is managing and using the information across the whole system. Our public health system is decentralized, with multiple entities making decisions. There are several information systems that have different functions and do not all talk to each other. On an everyday basis, the public health system does not need to have a robust information system tracking millions of products to their final destination for rapid response to changing supply and demand. There are also some new information systems being deployed; this could be helpful or it could add to the complexity.
We are already seeing misinformation campaigns, and there are documented concerns around vaccine hesitancy.
Another challenge is people. Namely, how do we reach people, including in fair and equitable ways? How do we make sure that people have trustworthy information about safety and efficacy?
We are already seeing misinformation campaigns, and there are documented concerns around vaccine hesitancy. The people managing logistics systems should remember that human beings are the ultimate consumers. That means logistics should include humans in the loop in multiple ways to support equitable, just outcomes that take into account patient opinions.
TA: Why do some COVID-19 vaccines have to be kept ultra-cold?
Swann: These are the first mRNA vaccines authorized for widespread use! Scientists have been working for more than a decade to get to this point. Messenger RNA (mRNA) provides a set of instructions to your cells. To get into the cells, it is encased in a lipid fatty acid. The lipids need to be kept cold so they do not merge with each other, like M&M’s need a coating to not become a melted chocolate mess.
These vaccines do not include live virus, and they do not interact with a person’s DNA. The ingredients are known and have not generated concern.
There are also other vaccines being developed, with several types of technologies. The Johnson & Johnson vaccine is built on an adenovirus (like its recent Ebola vaccine), and the Novavax one on a protein (like its candidate flu vaccine, Nanoflu). [Editor’s note: we discuss how these various vaccines work at greater length here.]
The temperature for a particular vaccine can be specific, based on its specific formulation and the testing that the company has done to show stability. The Ebola vaccine distributed in West Africa also needed to be kept very cold, which was done through a combination of freezers and a new type of thermos.
TA: What is being done, that we know of, to address all of these challenges?
Swann: We have known for months about the scale, and certainly everyone in the country has become aware that supply chain disruptions can have negative impacts. So people have been working on developing solutions. Pfizer and Moderna have been testing the vaccines to allow for relaxation of temperatures in ways that maintain the vaccine stability and potency. Massive educational campaigns have already begun to address vaccine hesitancy.
Also, the National Academies of Science, Engineering and Medicine report on allocating vaccines, and recommendations from the CDC’s Advisory Committee on Immunization Practices recommendations, are important steps toward beginning to address issues around inequities and disparities in outcomes that have already been occurring. We have also seen a number of companies who are innovating to solve problems, including the development of mobile freezers, ultra-low cold devices, forecasting systems and others.
TA: The rollout of the vaccination program has been slower than many people were hoping. What have the stumbling blocks been, and do you think things will speed up soon? [*This question was added on Jan. 6, 2021.]
Swann: The rollout has been slower than we would like, and there are multiple causes.
First, the information available does not give authorities perfect knowledge, as we are told how many doses have been distributed (where there may be a 2-day delay until receipt within a state) and administered (where it may take 72 hours to get full reporting).
Secondly, I anticipate that vaccine administration will speed up since we are now past two major holidays.
Third, health departments have been taxed for almost a year with responding to the pandemic, and very few resources were made available to assist with the “last mile” distribution (meaning that final step before the vaccine reaches the consumer). That last mile is often the most challenging part of the supply chain. Resources could have supported people for planning and the support work for vaccination (which often requires more manpower than just the actual shots in the arm) as well as information technology systems to make the process more efficient.
There are other reasons, but I think it is more important to focus on what can we do to improve things. I anticipate that the pace of administration will increase as we expand beyond the initial priority groups to others, including allocating vaccine to additional sites for administration.
Health departments and providers are also learning from the experiences of others and tweaking the system, developing policies for when there is vaccine left at the end of the day that would perish or if supply is otherwise greater than the demand at a particular location. Large organizations, including employers and universities, should also be setting up information technology to support a smooth roll-out. This might include things such as pre-booking appointment slots based on priority group, and systematic ways to prevent fraud in who is receiving the vaccine. Like any other major task, planning is crucial, and if that planning is informed by what we’re learning today it will be even more useful.


